A medical device design that adds value to end user and simultaneously captures profitable market share is really a tough job.
The medical device space is a highly regulated and innovation-driven industry, which adds unique challenges to the design and development process.
Is it because healthcare is a life-critical segment? Or is it because it involves complex procedures?
Apparently, both. In addition, it needs to be aligned with healthcare regulatory requirements, solution specifications, and should deliver functionalities to satisfy end user needs.
Hence, it seeks a holistic approach to design a medical device rather than being an isolated part of the complete process. It requires precision in every stage — right from product ideation to compliance, designing, testing and marketing of the product.
Why is Medical Device Design Important?
Design and development of a medical device is the most crucial phase for its success. A loosely-defined and designed medical device cannot comply with the regulatory needs and make it to market.
Successful medical device design and development relies heavily on the expertise and collaboration within product development teams. These interdisciplinary teams, which include engineers, designers, and medical professionals, work closely together to ensure regulatory compliance and that the device meets market needs. Without this collaborative approach, even if a device passes compliance, it may fail to deliver the defined functionality and benefits, resulting in lower market adoption compared to well-designed products.
Spending hours with medical device developers and studying multiple Medtech projects, including allergic drug vending machine, software controlled insulin pump, endoscopy device miniaturization and much more at eInfochips, now I understand that medical device design and development is more than just conceptualizing a solution, developing a prototype and mass manufacturing to sell.
How to Design and Develop a Medical Device?
It takes a significant amount of effort to deliver the right healthcare solution that meets customer demands. A right healthcare solution demands everybody staying on the same page, with strong scope definition from end user’s need, collaborative efforts across the team, adherence to specification and requirements extracted from product definition, simultaneously mitigating risks and sticking to the best possible quality. Developing a robust regulatory strategy early in the medical device design and development process is essential to ensure smooth navigation of compliance requirements and to integrate regulatory considerations into every stage of product development. Considering these, here’s a comprehensive guide to designing and developing an effective medical device for Medtech professionals.
I am putting everything inside out in this definitive medical device design guide to successfully design and develop Medtech solutions and medical devices that address the needs of customers as well as serve the compliance needs.
Here is the index for the same:
- Product Ideation and Conceptualization
- Addressing Regulation and Compliance need
- Design control regulations
- Testing – Verification and Validation
- Risk management procedures
Let’s get going.
Product Ideation and Conceptualization
Like other industries, Medtech innovation starts with analyzing and identifying the market, the need of which is untapped or unmet or there is a more efficient way to address those particular needs. Involving medical professionals during the ideation and conceptualization phase is crucial to ensure that clinical needs and usability are properly addressed. These needs could be anything that delivers a solution such as a new or better way of monitoring health, enhanced care delivery solutions, devices or technologies to deliver better administration or anything that supports health and a human life.
These needs either could be “Vitamins” or “Pain Killers”.
Let us understand what are Vitamins and Pain Killers in terms of product development:
It’s not obvious that a device must address a particular problem, a device might also be a solution that aids convenience on a routine lifestyle or situation.
For an example: A device like health tracker tracks steps taken, calories burned or even monitors one’s sleeping habit. In this case, it doesn’t deliver a solution but gives you a fair idea about your daily routine, which helps you to improve health or lifestyle. This kind of solution is termed as Vitamins while a device that addresses a problem such an Insulin Pump is a Pain Killer.
Ideally, product ideation and conceptualization start with the following steps:
Step 1: Identification of Need
Identifying the need for demand is a primary step for creating a medical device offering, apart from being compliance-ready.
The success of this depends very much on two things:
- The gap between the need of target market and what Medtech developer perceives as the need; the lesser the gap, the better inputs for product definition
- A strong product definition extracted by analyzing the market needs
Most medical devices today incorporate software components, so it is important to consider software integration and requirements during the product definition phase.
(Hint: Medical device product definition is about defining design and desired performance with a specific need.)
Step 2: Device Classification
Once you are done with the product definition and idea, you need to consider procedures like FDA defined classification and intellectual property rights.
Medical device classification is based on the risk associated with the use and enforced by law. Moderate risk devices, typically classified as Class II, often follow the 510(k) regulatory pathway and require specific risk mitigation strategies during development. Also, you need to look for any pre-existing Intellectual Property on the proposed idea or similar; it might actually disallow you to use the mechanism or technology.
To carry out complete discovery phase, a strong development team is crucial. This may be a pitfall if the team is not well experienced. In any case, you can decide to go with an in-house team, a consultant or a company to get help with medical device engineering.
Whatever option you choose, the team needs to be experts in the following areas:
- Engineering and design
- Human factors and usability engineering
- Clinical and scientific knowledge of medical industry
- Regulatory affairs and quality assurance
- Intellectual property law
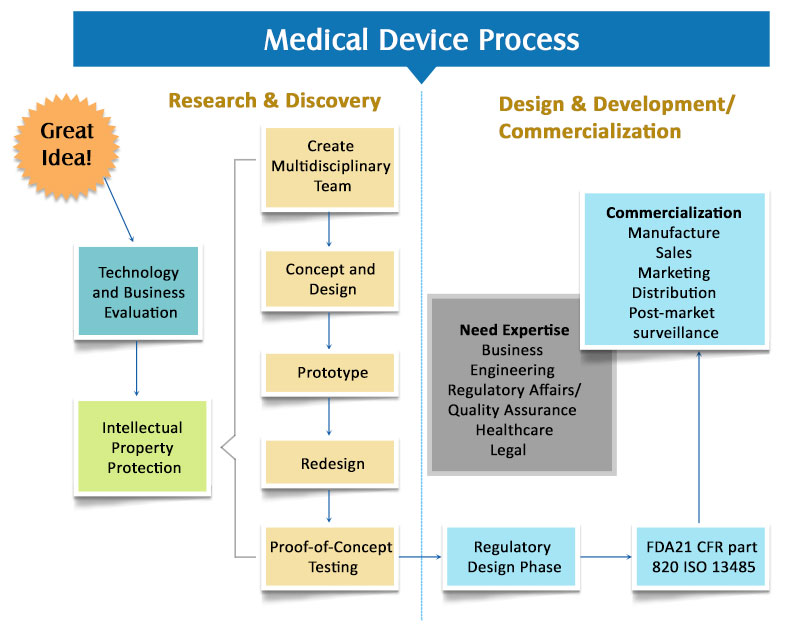
Step 3: Transition to Discovery Phase
The next step is to transmit the idea into the discovery phase. This phase consists of initial designing, prototyping, PoCs, and iteration driven redesign. For complex devices, this stage requires more detailed and structured planning, such as using comprehensive project management tools to manage their intricate components and regulatory requirements. Once you successfully complete the product conceptualization and discovery phase, you may proceed further for FDA approval and commercialization.
What are some Biggest Challenges in Medical Device Design?
What was science fiction 15 years ago is in FDA trial today. Mechanical engineers are dealing with new materials, electrical engineers are moving to new low-power chips, and software designers are migrating to new mobile operating platforms.
With these facts in mind, we surveyed 35 medical device designers and curated a whitepaper about what they think as medical device design challenges in future.
Addressing Regulation and Compliance Need
In order to get into the market, the medical device needs to pass through certain regulatory compliances, subject to both regional and international standards. Adhering to FDA regulations is crucial during verification and validation to ensure device safety, efficacy, and successful market entry. Medical device standards are helpful and enforced by law in specifying and evaluating the requirement for design and performance parameters for a biomedical materials, tools, and equipment.
These medical device standards allow institutions in the medical device field such as product manufacturers, laboratories, and others to inspect and assess such equipment and devices to ensure standard quality and usability.
International Electrotechnical Commission (IEC)
The International Electrotechnical Commission (IEC) published first of its kind medical devices standard in 1970, IEC 60601-1. IEC 60601-1, Medical electrical equipment – Part 1: Is the internationally recognized standard which addresses general requirements for medical electrical equipment and devices covering standards for basic safety and essential performance.
The IEC 60601-1 has undergone many revisions time to time over the years in order to remain adaptive and up-to-date with newer medical technologies. The latest set of changes was introduced with the 2012 publication of Amendment 1 to IEC 60601-1. This standard includes the requirements for essential performance, commands usability engineering evaluations and human factor consideration, and mandates the adoption of a formal development life cycle process for software.
It also specifies new as well as revised technical specifications for electrical and mechanical hazards, also new product labeling and documentation requirements.
International Organization for Standardization
The International Organization for Standardization also have specifications for medical device standards. ISO 13485 and ISO 14971 are widely used standards across the world for medical device quality management. These standards require thorough documentation and management of design and development activities to ensure regulatory compliance, as outlined in frameworks like 21 CFR 820.30 and ISO 13485.
Other than these international standards, there are certain standards which are region specific and all of them are adopted from international standards with little modification and limitation.
- If you are manufacturing or selling medical devices in the US, the medical device will be regulated by the Food and Drug Administration (FDA).
American National Standards Institute (ANSI) is the representative of ISO standards in the US. There are two more similar organizations: Association for the Advancement of Medical Instrumentation (AAMI) and the American Society for Quality (ASQ) that defines standards for the US.
If you have designed a device considering ISO standards, there is a possibility that the FDA may not approve the device. As FDA has its own set of procedures for risk management derived from both international and regional standards, which includes:
- ISO 14971:2007, Medical devices – Application of risk management to medical devices (international standard.)
- ANSI/AAMI/ISO 14971:2007 (R2010), Medical devices – Application of risk management to medical devices (A regional standard with additions and modifications from the referred international standard.)
In case of quality management standard, it does not follow the international or regional version of ISO 13485 standard. This is because FDA has different guidelines for quality management in medical devices for the US market.
- For the European Union, the European Committee for Standardization (CEN) is the standardization adopted from ISO and the European Committee for Electrotechnical Standardization (CENELEC) is the regional standard inspired by IEC.
CEN is a bit modified as per requirement from ISO and written with “EN” prefix. For e.g.:
- EN ISO 13485:2012, Medical devices — Quality management systems — Requirements for regulatory purposes
- EN ISO 14971:2012, Medical devices — Application of risk management to medical devices
National members adopt these standards from EU while adding their own prefix. For Switzerland, Swiss Standards publishes standard with “SN” as prefix such as SN EN ISO 13485:2012 and SN EN ISO 14971:2012.
- For Canada, Canadian Standards Authority (CSA) is the representative organization for ISO.
Looking for Regulatory Compliance Services?
At eInfochips, our experts provide HIPAA compliant engineering solutions, and have the required process expertise in IEC 60601-1/2/6, IEC 62304, 510K and ISO 13485.
Design Control Regulations
Medical device manufacturers need to follow Design Control guidelines since the regulatory bodies like FDA, European Commission, Health Canada, and others want to ensure that the medical devices are safe for potential users before manufacturers start to market the devices.
Like I said earlier, the FDA doesn’t follow ISO 13485 as it has different requirements for quality management. Design controls are defined under FDA 21 CFR 820.30 which has a similar intent to section 7.3 Design and Development described under the guidelines for ISO 13485.
Additionally, FDA incorporates Current Good Manufacturing Practice (CGMP) requirements into the quality system regulation with an aim to follow good quality practices for medical devices design. The regulation provides a framework to implement the design control to a wide variety of devices. The framework delivers flexibility for both regulatory compliances as well as internal design and development process. For class III medical devices, even more stringent design controls, verification, and validation processes are required due to their higher risk classification.
To successfully implement design control of medical devices, professionals with both technical and non-technical background, such as business administration, life science, engineering, computer science, and the arts are required.
Design controls guideline is a quality system approach that covers the entire life of medical device starting from design, production, distribution, use, maintenance, and obsolescence.
Here is the index for Design Control clause of the FDA.
- SECTION A. GENERAL
- SECTION B. DESIGN AND DEVELOPMENT PLANNING
- SECTION C. DESIGN INPUT
- SECTION D. DESIGN OUTPUT
- SECTION E. DESIGN REVIEW
- SECTION F. DESIGN VERIFICATION
- SECTION G. DESIGN VALIDATION
- SECTION H. DESIGN TRANSFER
- SECTION I. DESIGN CHANGES
- SECTION J. DESIGN HISTORY FILE (DHF)
Medical Device Design Control Process
Initial phase from which Design Control starts is Design Input development and approval, which consists of device design and manufacturing processes to be carried out in the production phase.
Design control is a holistic approach and doesn’t end with transferring the design to the production phase, once the design is finalized. It also impacts manufacturing processes according to the changes in the design phase or even post-production feedback. It is an ongoing process to develop a product that is usable for a user and thus for the enhanced product, it considers revolutionary changes from usage pattern as well as analyzing failed products.
The image below depicts how Design Control can be performed in the waterfall design process.
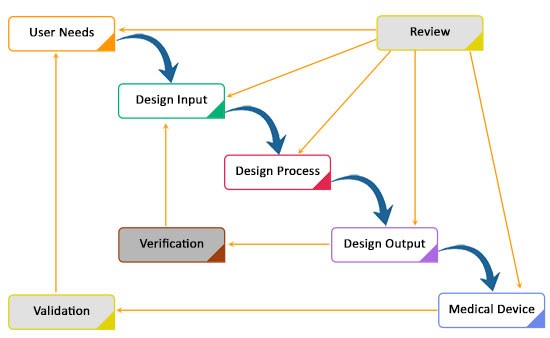
Step 1 (User Needs)
Requirements are defined considering the market need and the device is designed to address that need. After series of evolution, the medical device design is finalized and transferred to production for manufacturing. There is a need of feedback during each and every step of this process.
Step 2 (Design Input)
This is an iterative process. When an organization decides to address the particular need, they review and test the acceptability of design input derived from the need. At that point, the iterative process of converting requirements into device design starts.
Step 3 (Design Process)
These design inputs are converted into design output by converting those requirements into high-level specifications (which are Design Output).
Step 4 (Design Output)
Verification process confirms whether the specifications are satisfying requirements or not. And the output becomes the input to revise the requirements and this process goes on until Design Output is aligned with the Design Input. At this stage, detailed design specifications are essential for guiding engineering teams in prototype creation, testing, and manufacturing process development.
Step 5 (Medical Device)
Once the final design is ready, it is transmitted to the production facility for mass manufacturing.
Design control regulation mandates Design History File (DHF), which illustrates the linkages and relationships between all the Design Controls and help to trace all changes throughout the entire product development process.
You can take a paper-based approach or a software-based approach, especially developed for Design Control; your design history file must be traceable as well as accessible to all the team members.
Testing – Verification and Validation
Every medical device must meet the functionality, usability and reliability objectives to get a successful share in the market. Apart from these, end users also look for effectiveness and safety of devices that they use to address a particular problem or condition, which are sometimes critical to life. This is why iterative testing with verification and validation of these medical devices becomes imperative.
Verification and validation of medical devices in the design process aim to ensure that the device is aligned with the need of targeted users and it delivers the intended solution. It also helps ensure whether all the requirements are being satisfied or not. Rigorous testing and analysis during verification and validation are essential to ensure the device’s safety. It helps to comply with regulation as well as designing the highest quality product and manufacturing processes.
Verification is internal to internal process, which evaluates whether a design output meets the specified requirements, specification or regulation defined in the design input. Whereas validation is internal to an external process, which evaluates if your product delivers benefits, according to the need of targeted users or not. Clinical evaluation is a critical part of validation, as it assesses the device’s performance in real-world scenarios and helps mitigate risks associated with its use.
Medical devices may consist of different technology shapes, sizes, and different level of complexity. Verification and validation (V&V) activity is driven by regulatory environment and must follow international standards.
Standardized V&V activities can streamline the manufacturing process as well as enhance approval process. Additionally, automated testing, diagnostic techniques, and data collection tools can enhance the V&V process.
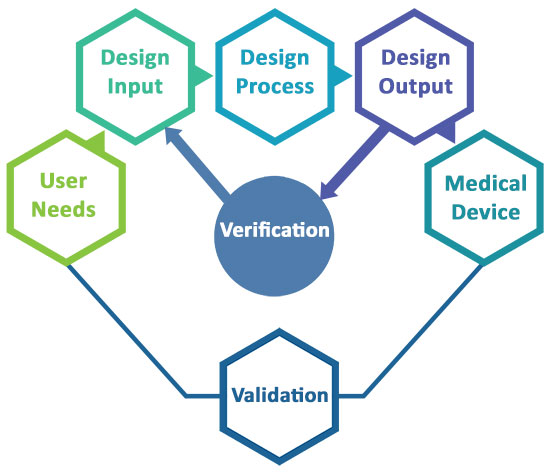
V&V being an iterative process consumes a lot of money, when planned poorly. A strongly-defined test strategy can help you optimize cost as well as the test period to make the product market ready on time.
The complexity of any testing strategy depends on technologies to be used and geographical target markets. The test strategy should cover at least six parameters mentioned below:
- Targeted geographies and associated standards
- Time to market
- A standard to be followed with version
- Testing Labs – internal or independent labs
- Defining the sequence of tests
- Presenting the test result
Accordingly, tests used for verification and validation process also needs to be validated. This is to ensure that you measure what you need to measure because a wrong test will deliver wrong outputs of usability and functionality. Medtech companies need an effective and well documented V&V, which complies with associated regulations. These processes are specifically designed to ensure patient safety in accordance with regulatory standards.
HANDPICKED RELATED CONTENT
Implementing Medical Device Testing Strategies: A High-Level Overview
Risk Management Procedures
Risk management procedures for medical devices are enforced under internationally accepted compliance standard ISO 149711:2007 Medical Devices – “Application of Risk Management to Medical Devices”. Apart from this, risk management policies need to be incorporated across all the stages of medical device design and development and should be also associated with design control aspects as well.
Effective risk management also includes monitoring and analyzing adverse events to identify safety concerns and improve device safety.
Why is risk management procedure important?
Considering the complexity of medical device design, focused risk management practices help ensure usability, safety, and regulatory compliance. It is a process of identifying, controlling and preventing the failure that may cause hazards to users. It also mandates identifying associated risks. Upon reaching an unacceptable level of risk, it notifies developers to decrease at least up to an acceptable level.
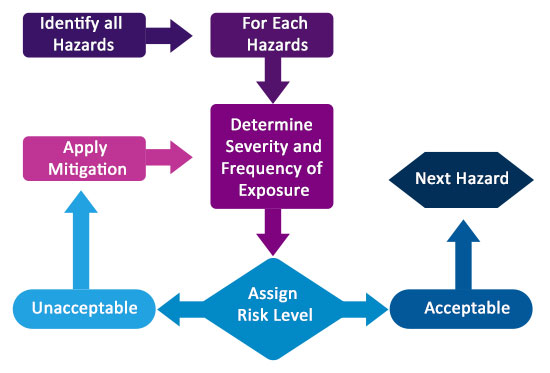
How is Risk Management Procedure Followed?
The above image shows all the steps involved in the risk management process. The process starts with the identification of hazards and then associated risk is measured based on the consequences of hazards and their possibility of risk.
If the identified risk level is above the defined criteria, then it needs to be mitigated. The risk level depends on many parameters such as the device, technologies or even company’s risk acceptability policy.
Before finalizing a design, it is good practice to conduct a hazard analysis to get an idea about the standard hazards associated with the device. Primary hazard analysis can be done easily by considering major components and operational requirements such as raw materials and wastes, hardware, monitoring and control systems, human-device interfaces and services; and then identifying potential hazards associated.
There are certain hazards that must be evaluated:
- Raw materials and wastes: toxicity, flammability, and reactivity of material
- Environmental factors: sensitivity to temperature and humidity and more
- Mechanical or electronic hazards
- User device interface: hazards associated with human factors like ineffective delivery, drug administration, incorrect or incomplete information, control of life-sustaining operations
When multiple hazards are identified, they can be prioritized according to severity associated with them. Often, there is a scenario where you have insufficient information to identify hazards. In such cases, you may consider similar devices and their history for identification purpose.
During the prototype development phase, there is a need for detailed hazard and risk analysis. There are two approaches for hazard analysis: Top-down and Bottom-up approaches.
- A hazard and operability (HAZOP) and Failure Mode Effects Analysis (FMEA) are analysis techniques with a bottom-up approach. HAZOP is ideal for complex design, which involves multiple step processes. While FMEA is ideal for devices having multiple mechanical components, it is time-consuming.
- Fault tree analysis is a top-bottom approach to identifying top-level undesired output by analyzing combination and a series of lower level events.
Biomedical Engineering and Device Design
Biomedical engineering blends engineering, creativity, and medical expertise to create innovative healthcare solutions. The medical device development process typically moves through six key phases—from concept to a safe, market-ready product. This journey involves human factors, risk analysis, and strict regulatory compliance at every stage. From ideation to testing and production, each step is focused on meeting the needs of both patients and healthcare professionals. Achieving approval from the U.S. Food and Drug Administration is a crucial milestone, ensuring the device meets high safety and performance standards.
Quality Management and Assurance
A strong Quality Management System (QMS) is essential to ensure consistent quality and regulatory compliance. Standards like ISO 13485 guide manufacturers in managing design, risk, suppliers, and CAPA processes. Embedding quality early in the design phase helps maintain safety, reliability, and consistency throughout the product lifecycle—building trust with regulators and end users alike.
Industrial Design and Development
Industrial design shapes how a device looks, functions, and performs. It combines usability testing, clinical validation, and material selection to ensure safety and effectiveness. A human-centered approach ensures devices are intuitive and practical, while balancing complexity, risk, and market needs. The goal is to deliver devices that are safe, compliant, and easy to use.
Conclusion
Every marketable medical device needs deep level engagement, considering the complexities involved due to the requirements, usage patterns, user experience, regulations, associated iterative process, technologies, material, and many more.
The final stages of medical device design and development involve manufacturing transfer, where the device transitions from development to production. For complex medical devices, this phase requires specialized expertise to manage regulatory submission processes and ensure all documentation, risk management, and compliance requirements are met. It is essential to obtain regulatory approval and achieve regulatory approval from authorities such as the FDA or EU before market entry. After launch, post market surveillance is critical for monitoring the device’s performance, ensuring ongoing safety, efficacy, and regulatory compliance throughout the product lifecycle.
To stay in line with competition or decrease time-to-market, you may need help from an experienced medical device engineering consultants or service providers.
If you want to explore more, here is the bonus research for you. We had asked 35 medical device developers on what is the most critical factor to the success of their medical device design, read here about what they think.









